On March 14, Mallory Pease woke with a sore throat but didn't worry much about it. Pease was nearing her second baby’s due date and knew that feeling rundown sometimes happens late in pregnancy. But then she became congested. Soon after, she couldn’t taste or smell anything.
“I was sleeping every chance I could get. I was also nine months pregnant so I didn’t really think anything of it,” Pease, 27, of Homer, Michigan, told TODAY. “Then the coughing started and shortness of breath.”
Later that week she had a fever. In the back of her mind, she had a nagging worry: What if it is COVID-19? But she thought that was unlikely: Even before social distancing and stay-at-home orders were the norm, she was already nesting at home and avoiding social gatherings.
A week after her first symptoms, her condition worsened and breathing was a struggle. By the time her water broke on Sunday, she was afraid.
“I was really out of breath,” she said. “I knew that there was no way I was going to be able to get through contractions and still find the energy to breathe.”
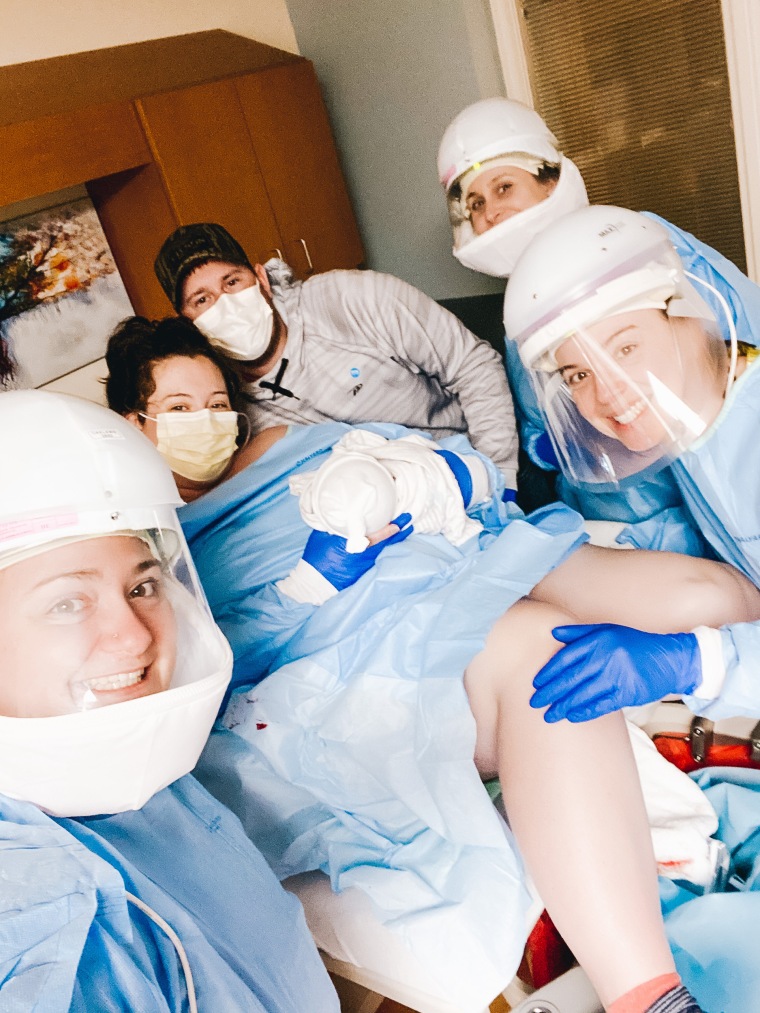
When she arrived at Oaklawn Hospital in Marshall, Michigan, she and her husband, Mitchell, immediately went into a room alone. Both had to wear masks and the labor and delivery nurse wore full personal protective equipment and stayed in the room the entire time. Doctors — also covered head to toe in PPE — tested Pease for pneumonia, flu and coronavirus, she said. While she immediately learned that she did not have flu or pneumonia the results of the COVID-19 test took longer.
“Deep down I knew I had it, but I still didn’t want to admit it,” Pease said.
While she hoped to deliver her daughter without an epidural, she quickly realized she needed relief. As she labored from midnight to 5 a.m. she took “shallow pant-like breaths” but often needed oxygen.
“That helped a lot,” she said. “It wasn’t bad until I needed to take a big breath. That is when I would start coughing and that would make me more out of breath.”

After Alivia was born doctors let Pease hold her for five minutes before she was whisked away to the isolation nursery and Pease went to the coronavirus floor. Alivia tested negative for it, but doctors still kept her under observation.
While little is known about pregnancy and coronavirus, one recent study found that pregnant women who have COVID-19 may be able to pass the infection onto their babies. It is unclear if that transmission can occur in the womb.
While Alivia was under observation, Pease became sicker. She spiked a fever and often gasped for air.
“I could hardly stand up to go to the window. I had to get help to go to the bathroom. And I needed somebody to help me get unplugged from everything,” she explained.
As coronavirus spreads across the country, more women are experiencing pregnancy and labor with it. The uncertainty of the novel coronavirus brings new challenges to pregnancy.
Beth, 33, a freelance wedding planner in New York City who asked not to use her last name, is pregnant with her second child due May 16. Nearly a month ago, she stared having symptoms, including shortness of breath, weakness and chest pains. When she first asked about it, her doctor suggested she was having a panic attack.
“They weren’t as supportive about my symptoms without a positive test as I would have preferred them to be. That has probably been the most difficult part. My primary care doctor can’t exactly recommend certain things because I’m pregnant. Then I turn to my OB and they are saying to call my primary care doctor,” she told TODAY. “You end up just trusting your gut that you’re going to survive and get through it.”
Her husband, Mike, and 2-year-old daughter also experienced coronavirus symptoms and after Beth’s throat swelled up, she finally received a test and learned she was positive. While she is feeling better after 25-plus days of symptoms, she’s worried how her status will impact her ability to go to the rest of her prenatal appointments. So far, most of them have been video checkups.
“They said they prefer for me not to come in,” she said. “It has been really stressful. I just keep worrying what if there is something wrong with the baby and I have to go and been seen and then I am putting people at risk.”
While Beth hasn't required hospital care to treat her coronavirus symptoms, Pease required a longer hospital stay than having a baby normally requires. A few days after giving birth, she was finally able to breathe without supplemental oxygen.
“I was still out of breath and it took me a while to catch my breath,” Pease explained.
On Thursday, March 26, she returned home while Alivia went to stay with an aunt for a week to allow Pease to recover. She needed the help, too. Just cuddling her baby drained her.
“Just sitting and holding her and nursing, as much as we could do it, was just completely exhausting,” Pease said. “I had zero energy so that was a wake-up call.”

Alivia is at now home with Pease, Mitchell and their 2-year-old daughter, Emma, and Pease feels better each day. Over the weekend she had a bad night of sleep, which caused coughing fits.
“I still need to take it slow and not rush this healing process,” she said. “Our story has a happy ending. I want people to know it’s not all bad but coronavirus is not something to take lightly.”
