Riley Ickes, a soft-spoken 16-year-old in Akron, Ohio, was always the bigger kid. As a toddler, Ickes began seeing doctors to figure out what was causing her rapid weight gain, but no one ever had answers. Many of them just assumed her parents were overfeeding her. By the time Ickes reached sixth grade, the scale was hovering around 250 pounds.
“I tried every diet you can possibly think of but nothing worked for me,” Ickes told TODAY Health. “I was exhausted from trying."
At age 13, Ickes began seeing specialists at Healthy Active Living, a weight management clinic at Akron Children's Hospital. It was there that she learned about bariatric surgery.
"They thought I was a good candidate," Ickes recalled. "My dad struggled with it a little bit at first, just because he didn't know much about it. But I knew it was something I wanted to do."
In September 2020, Ickes, who at her heaviest weighed 324 pounds, had bariatric surgery at the hospital. Ickes describes her recovery as "great and painless." She took off two weeks from school.
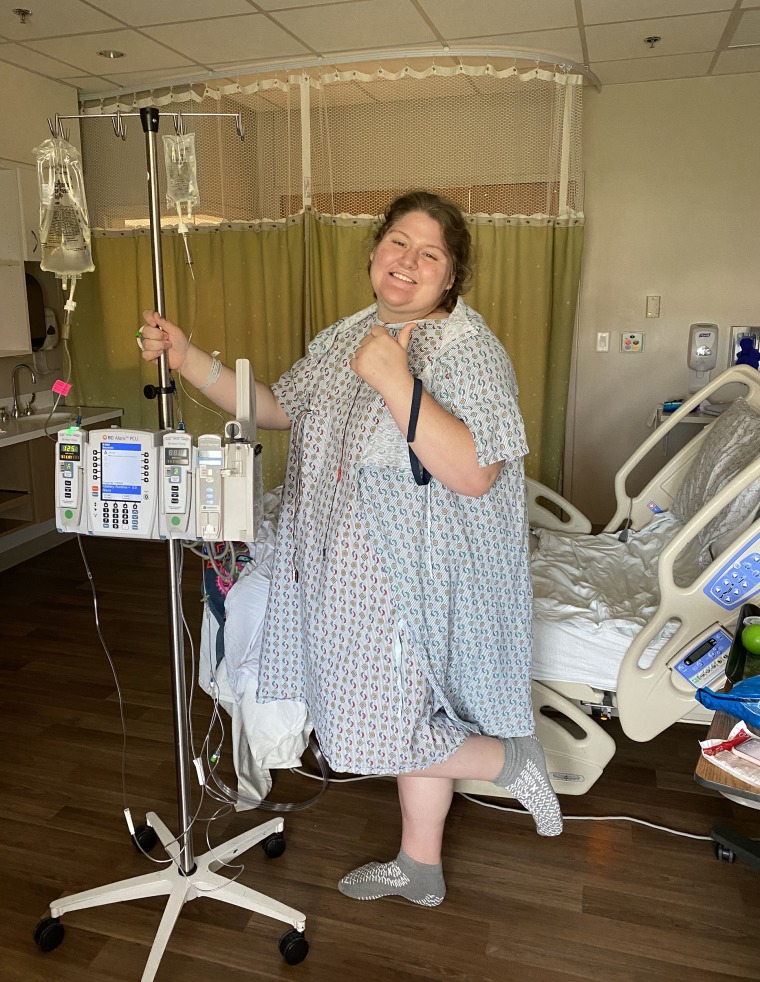
In less than six months, the high school junior has lost more than 100 pounds after undergoing a vertical sleeve gastrectomy (VSG), a laparoscopic operation where a portion of the stomach is removed. The surgery also reduces hunger by eliminating the portion of the stomach that produces ghrelin, the hormone that stimulates appetite.
Ickes, who has polycystic ovary syndrome (PCOS), a hormonal disorder which is associated with being overweight, no longer suffers from prediabetes or high cholesterol levels. The physical changes are astounding — but so are the emotional ones.
“I used to struggle with so much anxiety. I hated when attention was on me,” Ickes revealed. “I never in a million years thought I could feel this good or happy.”
Ickes's mom, Renee, echoed the sentiment.
"Riley dances around the house now," Renee said. "She's a different person."

Bariatric surgery for kids: What parents should know
The American Academy of Pediatrics (AAP) believes all children deserve the same treatment option that Riley was offered. With severe obesity affecting nearly five million U.S. kids, the AAP issued a policy statement in December 2019, advocating for greater access to pediatric bariatric surgery, which is proven to be both safe and effective.
According to Dr. Sarah Armstrong, who served as the lead author for the AAP policy statement and is division chief of general pediatrics and adolescent health at Duke University, there is no minimum age for the irreversible procedure.
Children are eligible for surgery if their body mass index (BMI) is 40 or higher, or at least 35 if they have comorbidities such as fatty liver disease and diabetes. A BMI of 30 and above is considered obese according to the Centers for Disease Control and Prevention. When a person has a BMI greater than 35, their chances of reaching a normal weight for a lasting period of time is less than 1%, according to the American Society for Metabolic and Bariatric Surgery (ASMBS).
“There used to be concerns that surgery before puberty would interfere with growth, but there is no evidence to support that. In fact, obesity itself interferes with growth,” Armstrong told TODAY. “A second concern is the child’s emotional capacity to make such a big decision. That’s why we recommend the involvement of a child psychologist.”
Data that goes back roughly three years shows that most kids lose about 20 to 25% of their excess body weight and keep it off after surgery, Armstrong said. But according to a 2018 study, only 0.04% of children and adolescents with severe obesity have bariatric surgery, demonstrating a lack of access to and knowledge about the procedures.
“The insurance companies have not really moved their policies for coverage,” Armstrong noted. “And that’s a big problem.”
Dr. Mark Wulkan, chair of the Department of Pediatric Surgery at Akron Children’s Hospital agrees with Armstrong.
“Obesity is a disease,” Wulkan told TODAY. “The kids that come to us need help. Would you deny treatment to a kid with cancer? Would you deny a kid with diabetes their diabetes medicine? So if they have the disease of obesity, why should we not treat them?”
A life-changing procedure
It's been six years since Armstrong’s former patient Faith Newsome, 23, underwent gastric bypass. She is now studying obesity in graduate school and runs OCEANS Lifestyles, a bariatric support and advocacy group for teens.

“People love to simplify obesity. They say, ‘eat less, move more and you will lose the weight,’” Newsome told TODAY. “But obviously, I had tried that and it wasn’t working. I felt like something was wrong with me. I felt out of control — and I don't anymore."
Newsome has regained some weight, but she no longer suffers from hypertension and prediabetes. Her blood work is "perfect."

“I fluctuate between a size 12 and a size 16,” Newsome explained. “However, I’m no longer at war with my body — we’re on the same page. I'm healthy and I take care of myself."
For those interested pediatric bariatric surgery, Wulkan advises reaching out to your primary care provider and asking questions. Armstrong said that these conversations shouldn't wait.
"We often think of bariatric surgery as that last option. It's that thing that we'll do when everything else has failed," Armstrong said. "Unfortunately, that sometimes leads us to just delay into the point where a child's obesity is now very severe and the health damage has been done. We know that surgery is actually more safe and effective when the obesity is not as quite as severe."
Ickes, who will celebrate her 17th birthday next month, is looking forward to her future. She now works out five days a week and plans to start training for a marathon. Ickes's mom, Renee, raves that her daughter is now an expert at reading food labels.
"Check in on me in a few years," she told TODAY Health. "I'll still be going strong."
CORRECTION (Feb. 25, 2021, 12:53 p.m.): An earlier version of this story misstated the name of Faith Newsome. She is Faith Newsome, not Newsom.