This week Sen. Kamala Harris introduced legislation that puts a spotlight on a painful health problem that disproportionately affects Black women: uterine fibroids.
"We don't talk nearly enough about uterine fibroids, which affect millions of women across the U.S.," the California senator wrote on Twitter on Thursday, adding that her bill would help fund crucial education and research.
Fibroids are noncancerous growths in the uterus, which can cause painful periods for women, among other health issues. Harris is working on the bill with congresswoman Yvette Clarke, who has dealt with fibroids herself, even undergoing a related surgery in 2007.
"This disease has ravaged the lives of women across the country, and increasing funding for research and public education related to fibroids is critical to reversing that trend," Clarke said in a statement on Harris's website. "If we are serious about fixing inequities in our health care system, then we must treat uterine fibroids with the funding and attention it deserves."
Suffering in silence for too long
Many women say their lives have been seriously affected by fibroids.
Britt Julious remembers going to the nurse’s office in high school and joining the rows of girls lying on cots. They weren’t there because they had a cold or the flu. Like Julious, they were there because of their periods.
“It’s hard to be 15 or 16 years old and you’re trying to pay attention in algebra, and all you can think about is how you want to puke,” Julious, a 32-year-old writer in Chicago, told TODAY last spring.
“I would come home from school because I couldn’t function. I couldn’t sit up in my chair.”
Julious was only 10 years old when she got her period. Soon after, intense cramps began and continued throughout her adolescence into adulthood, when she learned she had uterine fibroids.
Painful periods are a symptom of fibroids. But for many women, pain alone isn’t reason to see a doctor. In fact, numerous women told TODAY they were taught that pain is simply part of being a woman.
Now a new wave of doctors and organizations want to tell people that’s not true.
But first, what are fibroids?
Fibroids are benign tumors in a woman’s uterus. They’re most common during a woman’s childbearing years, but can develop at any age. Fibroids can be as small as a seedling or bigger than a grapefruit, and women can have one, two, three or many.
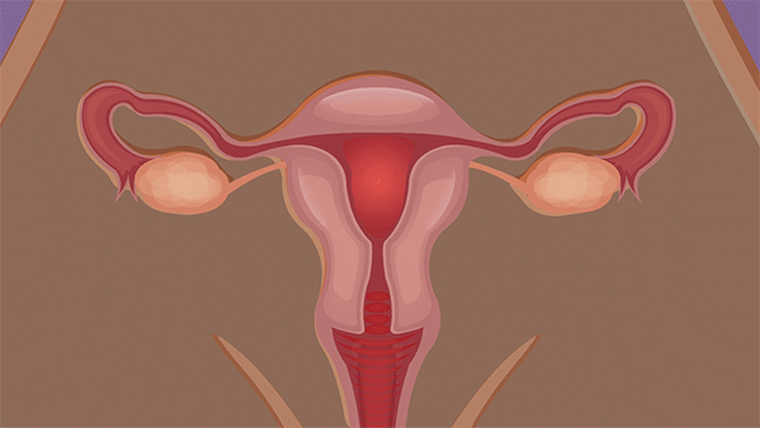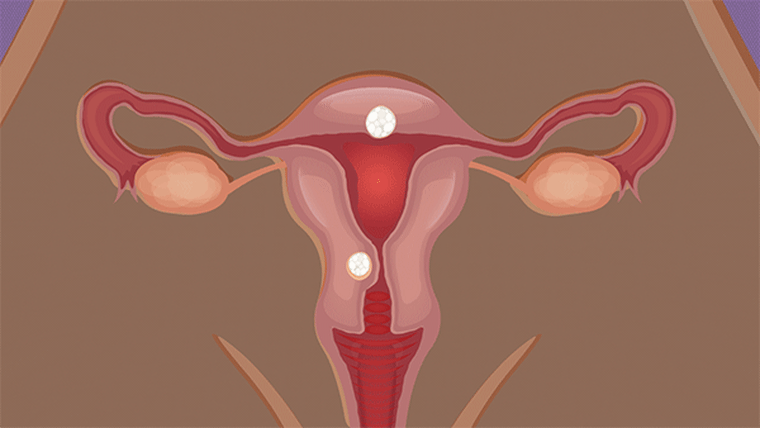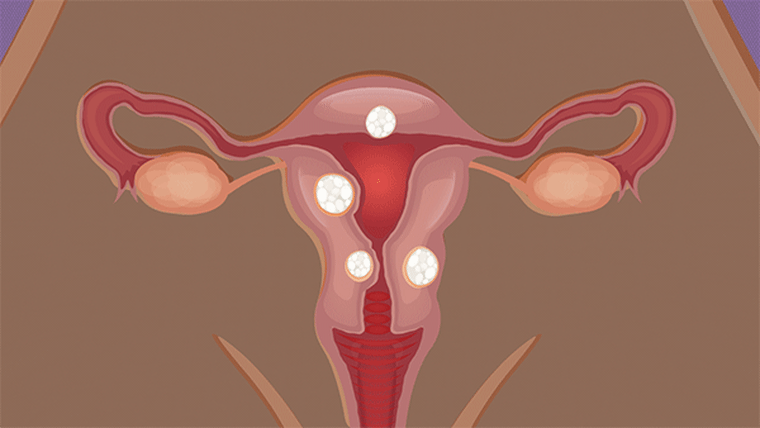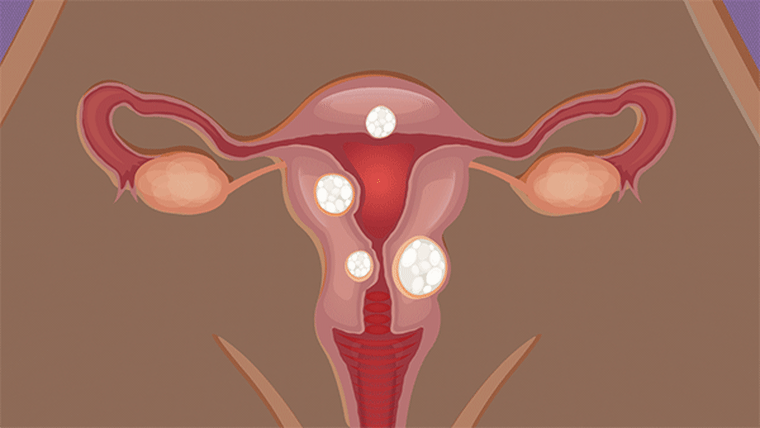
Fibroids are common but doctors do not know why some women develop them. Genetics play a factor: Women with a family history of fibroids are more likely to develop them. And Black women are especially at risk. Up to 80% of Black women will develop fibroids before they turn 50, and up to 70% of white women will develop fibroids before they turn 50, according to research. For Black women, fibroids are often more severe and occur earlier, according to Dr. Elizabeth Stewart, a fibroids specialist and professor of obstetrics and gynecology and surgery at the Mayo Clinic in Rochester, Minnesota.
While fibroids themselves aren’t usually life-threatening, they can definitely make women miserable. Symptoms include longer and heavier periods, intense menstrual cramps, digestive issues and pressure or bloating in the abdomen. Fibroids can also impact a woman’s fertility if they distort the cervix or uterus, although other causes of infertility are more common and many women with fibroids have no trouble getting pregnant, according to The American College of Obstetricians and Gynecologists.
“You’re conditioned to believe it’s normal.”
Experts agree there’s not enough awareness around fibroids. Part of the problem is the lack of medical research. Another part is the culture around women’s periods and women’s pain.
“It’s just not something women, especially women of color, talk about in their families,” said Evette Dionne, 30, a magazine editor in Denver, Colorado, during a phone call last spring. “If you’re having a heavier period or a painful period, it’s something that you’re conditioned to believe is normal. And so it doesn’t immediately register that it’s something that should be alarming to you.”
That creates a dangerous cycle, according to Stewart.
“There’s new research suggesting that maybe even the fact that (fibroids are) so common means that women don’t recognize they have a medical condition,” she said. “So if you’re having menstrual bleeding for ten days a month and you ask your mother and your sister, ‘Is this normal?’ and they have the same thing, they may say, ‘Yeah, this is normal.’ So even if you do talk about it, you may not get the correct information.”
In November 2018, a Twitter thread of Dionne’s about fibroids and how Black women need to advocate for themselves went viral, prompting dozens of other women to share their stories.
Dionne had one fibroid removed in 2015 and another five removed in February 2019. Many women in her family have dealt with fibroids — though she didn’t learn about her family history until after her own fibroids became a problem. She knew something was wrong about four years ago, when her menstrual cycles grew excessively long, sometimes lasting up to three weeks.
Julious had a similar experience with her family, and believes that Black women in particular are sometimes taught that their pain does not matter.
“We’re really taught to accept pain in a number of different forms,” Julious said. “You’re told to push through it, to ignore it. When you are in this world where you have to fight against racism, fight against sexism, fight against all these different things going on … you learn that whatever physical pain you’re feeling does not ultimately matter in the grand scheme of things.”
You learn that whatever physical pain you’re feeling does not ultimately matter in the grand scheme of things.
Britt Julious
Dr. Charles Ascher-Walsh, the director of gynecology and urogynecology at Mount Sinai Health System in New York City, added that because fibroids aren’t, generally, killing women, they may not get as much attention in the medical community as something like breast cancer, for example.
“It’s just not a sexy topic right now, so it’s not discussed that often,” he told TODAY. “It’s something that a lot of women suffer with for a long time. It’s sad to see.”
Of course, not every woman dealing with severe period pain, known as dysmenorrhea, has fibroids. They could have endometriosis or adenomyosis, for example. But the prognosis isn’t much better for those conditions. (Woman on average suffer with endometriosis for at least 10 years before they’re diagnosed, according to the Endometriosis Foundation of America.)
“Menstrual pain or pelvic pain in women is the only type of pain in medicine that’s described as normal,” said Sateria Venable, founder of The Fibroid Foundation, an organization based in Bethesda, Maryland, that aims to increase awareness of the condition. “When you have that as a data point, that sets the tone for sometimes dismissing (women’s) pain.”
A hysterectomy? Not so fast
Completely removing the uterus, or having a hysterectomy, is the only definite way to get rid of fibroids forever. But there are many alternative procedures to remove or shrink fibroids, as well as hormonal birth controls and lifestyle changes that may provide relief. The problem is that doctors aren’t always offering them.
Brooke Summers, a radio deejay in Kentucky, was told by three doctors that a hysterectomy was her only treatment option after being diagnosed with fibroids.
“I know I’m 42, but I wanted to keep all my body parts for as long as possible,” she told TODAY last spring. “Finally I found a female surgeon in Nashville who said, ‘It doesn’t matter the size, most likely I can just take out the fibroid, unless you want to have a hysterectomy.’”

She had a myomectomy earlier this year, a surgical procedure in which a fibroid is removed from the uterus wall, keeping her reproductive organs intact. Her fibroid was the size of a newborn baby. “I feel a thousand times better,” she said, although she is still recovering from the procedure.
The downside to a non-hysterectomy treatment is that the fibroids can always grow back. And certain procedures, like myomectomies, can be more complicated than a hysterectomy, which is fairly routine. (After cesarean sections, hysterectomies are the most frequently performed surgical procedure among U.S. women of reproductive age.)
“The average gynecologist does around 11 major surgical cases a year, which isn’t a lot,” said Ascher-Walsh, who operates up to 500 times a year. “So when somebody who doesn’t do a lot of surgery is faced with doing a surgery and they don’t know a lot of alternative options, and those alternative options are actually harder … you don’t offer them that, which is a horrible way to practice medicine, but it definitely happens.”
He added that for many women with fibroids, treatment could be as simple as going on birth control pills or getting a hormonal IUD, which can help control heavy bleeding. Women who find out they have fibroids should not wait until they're symptomatic to take action. Experts point to research suggesting that both vitamin D and green tea extract may help suppress fibroids.
“There are a lot of alternatives that women don’t often hear about,” Ascher-Walsh said.
Part of Venable’s goal with The Fibroid Foundation is to help women who want to preserve their fertility and avoid a hysterectomy by connecting them to doctors who are skilled fibroid surgeons.
“Not every gynecologist is capable of doing a successful fibroid surgery,” she said. “So many times, women don’t know who can help them.”
"I'm looking for relief — anything that will help me."
In July 2018, Julious underwent a radio frequency thermal ablation procedure to remove her fibroids. The procedure involves inserting a needle into the fibroids and using radio frequency energy to destroy the tissue. Unfortunately, the procedure didn't work, which is rare but possible. One of her treated fibroids has even grown since the procedure.
"I'm sort of like, 'Well, what happens now?'" said Julious, who also has ovarian cysts and thoracic endometriosis (endometrial tissue found in or around the lung). "I went through this costly, invasive, depressing, debilitating surgery, so what happens now? What should I do? And no one had any answers."

Julious, who works as an editor at Cancer Wellness magazine, recently started getting acupuncture and taking Chinese herbs. She's also found that when she follows a healthy lifestyle and diet, she feels better.
"At this point, I'm looking for relief — anything that can help me," Julious said.
Look at the number of drugs that have been developed for erectile dysfunction compared to the number of drugs that have been developed for fibroids, there's a big gap.
Dr. Elizabeth Stewart
There is some research that links diet to fibroid risk. But doctors still don't have a thorough understanding of why that is, and most experts say they need more studies to really understand the risks and benefits of the various treatments available for fibroids.
"The fact that there is so little research is an important point," said Stewart. "And that's true for many gynecological diseases. When you look at the number of drugs that have been developed and marketed for erectile dysfunction compared to the number of drugs that have been developed and marketed for fibroids, there's a big gap."
Venable, for one, is optimistic about the future for women with fibroids. She said that she's already noticed how people's attitudes around taboo topics like pelvic health and period pain have been starting to change.
"I think people are realizing how critical this is," she said. "I remain encouraged because ... I see how more folks are receptive and taking an interest in fibroids, and that encourages me greatly. Because that would not have happened 11 years ago, when I started this."
This story was originally published on May 9, 2019. It was updated with the news of the senator's legislation on July 31, 2020.

