In early October, 9-year-old Joey Pellegrini contracted COVID-19. Thankfully, his symptoms were mild and he was back in school about two weeks later. "All of his symptoms were over, the head cold had gone," Joey's mom, Jane Pellegrini, told TODAY. "We thought, 'No big deal. COVID wasn't that scary after all.' And that was it."
But a few weeks later Joey developed multisystem inflammatory syndrome in children, a rare but serious complication of COVID-19. As the name suggests, MIS-C affects multiple systems in the body and can even lead to organ damage or death without adequate treatment.
Experts have learned a lot about t and how to treat it since the beginning of the pandemic. And they told TODAY that the authorization of COVID-19 vaccines for use in younger groups of kids is a promising development. But as Thanksgiving and the winter holiday season approaches, there's concern that a recent jump in COVID-19 cases in kids could signal more MIS-C cases down the line.
Coronavirus cases among kids are still down from their peak in September, but have been slowly rising again since the end of October. In the week ending in Nov. 18, there were nearly 142,000 cases in kids, according to data from the American Academy of Pediatrics, which is up from 122,000 cases the previous week. And in some states, including New Jersey and Tennessee, MIS-C cases are increasing as well.
For Joey, MIS-C meant an emergency five-day stay in the hospital and lingering fatigue. Now, Pellegrini is sharing her family's story in the hopes that other parents will know what to look for — and act quickly — should their child develop signs of MIS-C.
The warning signs
On Oct. 29, Joey started feeling sick again with what Pellegrini assumed was simply a stomach bug. As his fever began to rise to about 103, she started to get more concerned. And on that Sunday, when his heart began beating so fast that his body was vibrating, she knew something was seriously wrong. "I went and got my Apple Watch and put it on his wrist," she said. "He had a really high heart rate of, like, 155 beats per minute."
The pediatrician's office was completely booked and nearby urgent care centers didn't have any openings until the evening. "My husband took the kids trick-or-treating and I took him to urgent care thinking we would be back in a couple hours," Pellegrini said. But the provider at urgent care was concerned about his EKG and sent them to the local hospital. After their blood test results came back, the two were sent by ambulance to Massachusetts General Hospital in Boston, about an hour away from their home in Fremont, New Hampshire.
"They had him hooked up to all the monitors, they had his IVs going," Pellegrini recalled, adding that he had to wait about six hours for a room in the pediatric intensive care unit. "From that point on, he spent three days in intensive care and then two days on the regular pediatric floor before we were released."
During his time in the hospital, Joey received his MIS-C diagnosis and was treated with intravenous immune globulin (a type of blood-derived antibody treatment), steroids, blood pressure medication and intravenous fluids. Doctors performed echocardiograms — essentially ultrasounds of the heart — and constantly monitored Joey's heart rate.
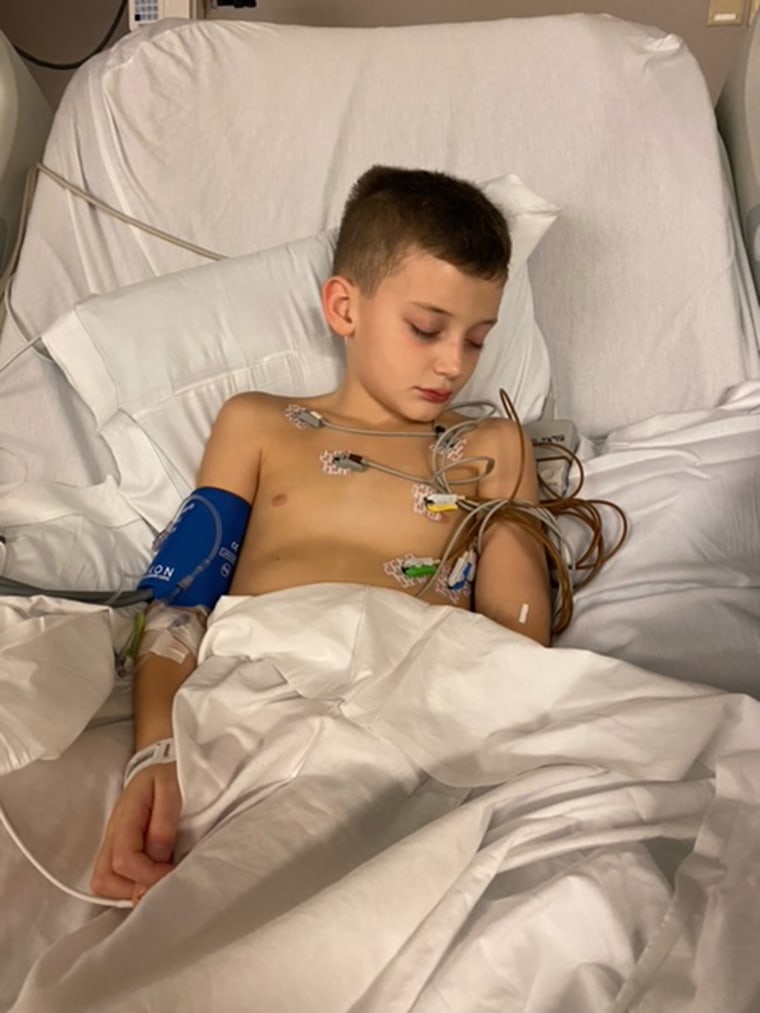
"I was completely unaware of this MIS-C. I had no idea to even look for symptoms," Pellegrini said. "If I had any knowledge of this, I would have brought him in at the first signs of the stomach bug."
What parents need to know about MIS-C
"We're now beginning to see an uptick again in (COVID-19 cases in) children, and children almost always follow adults," Dr. Diana Bianchi, director of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, told TODAY. "The concern is always that MIS-C tends to follow upticks in SARS-CoV-2 cases by three to four weeks."
There have been more than 5,500 MIS-C cases and 48 deaths due to the syndrome in the U.S. since the pandemic began, according to the most recent data available from the Centers for Disease Control and Prevention.
Although CDC data indicate that cases of MIS-C have been especially low over the past few weeks, that reduction is mainly due to a gap in CDC data on the syndrome. So experts can't say with certainty whether or not the current increase in coronavirus cases will lead to more MIS-C cases later on. But we shouldn't take the lack of MIS-C cases in the data right now as a sign that they aren't out there. The researchers that Bianchi works with across the country "have told us that they're seeing plenty of cases of MIS-C," she said. "So it's a false reassurance."
The condition typically affects children between the ages of 5 and 12 who initially had mild coronavirus infections, Dr. Adrienne Randolph, senior associate in critical care medicine at Boston Children's Hospital and professor of anesthesiology at Harvard Medical School, told TODAY.
Most of these children have minimal to no COVID-19 symptoms, explained Randolph, who has authored several major studies about MIS-C since the pandemic began. "And then approximately three to six weeks later they present with gastrointestinal symptoms like nausea, vomiting, abdominal pain, along with fever and a rash," she said. "About half of them present in shock and need to be in the intensive care unit."
At first, MIS-C might look like a case of gastroenteritis, Dr. Sandy Hong, pediatric rheumatologist and clinical professor of pediatrics at the University of Iowa, told TODAY. But with MIS-C, "they don't get better after a couple of days. They actually get sicker and sicker," she explained. The syndrome might also cause abdominal pain severe enough to look like appendicitis, Bianchi said. She noted that a few early cases of MIS-C actually resulted in unnecessary appendectomies.
If a child had COVID-19 and develops issues such as diarrhea, vomiting, lack of appetite, abdominal pain and persistent fever a few weeks later, that's certainly something to keep an eye on. However, Hong said she's seen kids with MIS-C whose parents didn't know they'd had COVID-19. Doctors may also be able to use antibody tests to help figure out if a child might have had a past coronavirus infection even if they never tested positive, Randolph explained.
Remember that MIS-C is generally rare. (The most recent estimates are that it occurs in somewhere between 1 in 1,000 and 1 in 3,000 cases depending on which set of statistics you're working with, Bianchi said.) But if your child has symptoms like those of MIS-C and you're worried, you should get in touch with your pediatrician — whether or not they've tested positive for COVID-19 in the past few weeks. And if those symptoms aren't improving after three days, that's when the AAP guidelines indicate the doctor should consider MIS-C.
Experts know more about how to treat MIS-C now, but still have unanswered questions
At this point, there is a standard model of treatment for MIS-C based on experts' understanding of Kawasaki disease, a similar sudden-onset inflammatory condition that affects young children. If a child has milder symptoms, they might just need to be monitored, Randolph said. But at the more severe end of the spectrum, typical treatment at the hospital might include IVIG and steroids like Joey received.
But researchers still don't know exactly what's causing MIS-C or why it seems to affect some children and not others. In some cases, genetics may play a role, Randolph said. In fact, her research suggests that kids with certain genetic markers may be more susceptible to the condition, she explained. But not all kids with MIS-C show those markers.
Additionally, the syndrome has some features in common with what experts call a "cytokine storm," which is an intense immune system response involving a type of protein called cytokines that's sometimes seen in autoimmune diseases. That's why, if a patient doesn't respond to IVIG or steroids, they might also receive biologic therapies that can dampen the body's overactive immune response, Hong explained.
Another factor that remains unexplained is why so many of the kids who've developed MIS-C (60% of those for whom ethnicity data is available, according to the CDC) are Black or Hispanic, Randolph said. That might be because people in those groups are seeing higher rates of COVID-19 overall, she added, but it's not clear.
Experts also don't know how COVID-19 vaccines — now available to kids as young as 5 — might change MIS-C rates. "If they're fully vaccinated, they won't get COVID. So therefore, by definition, they should not get MIS-C either," Bianchi said. "So if you're a parent and you're terrified about your child getting MIS-C, you can do something about it."
While the vaccines in teenagers are highly protective against acute COVID, Randolph noted that it's "really unclear" at the moment whether or not they can protect against MIS-C. "The hope would be that, as more and more children get vaccinated, the frequency of acute COVID will go down and also the frequency of MIS-C will go down," she said. But there isn't enough data to know conclusively if that's the case yet. That's a major question that ongoing research will hope to answer.
Other research projects are aimed at helping to diagnose MIS-C earlier on in the disease progress as well as figuring out which children are most vulnerable to developing the condition, Bianchi said. The Prevail Kids program, which the NICHD leads, is funding eight groups of investigators right now working with collaborators around the world on COVID-19 in kids and MIS-C. "They are working with blood, they're working with saliva, they're working with electronic health records," she said, in order to find patterns in childhood COVID-19 cases as well as potential biological markers that can be used to predict who'll develop the syndrome.
What is recovery like?
The vast majority of children who get COVID-19 do not develop MIS-C. And the vast majority of children who develop MIS-C are able to recover. But experts are still learning what kind of long-term effects kids who've recovered from the syndrome might experience.
Because MIS-C can lead to myocarditis and shares so many similarities with Kawasaki disease, which causes inflammation of the coronary arteries, "the biggest concern here is the heart," Randolph said. But other organ systems can be involved as well, including the neurologic system. So, what recovery looks like may depend on each patient's individual situation.
These days, Joey is recovering well at home. "His cardiologist cleared him to return to school as long as he is ready — with limited activity," Pellegrini said. "He will not be able to do gym class, no running around at recess." And while he's been able to continue schoolwork remotely, his energy levels are still low, she added.
He'll have to stay on steroids and blood thinning medication for the next few weeks and he'll have to take it easy for the next few months. But his mom is grateful that he's okay — and she wants other parents to be aware that, while rare, MIS-C can happen. "He's a totally normal kid and now he has to sit on the sidelines while other kids play on the monkey bars," Pellegrini said. "But in the bigger picture, I'm thankful that's all he can't do."
CORRECTION (November 24, 2021, 2:00 p.m.): An earlier version of this article misstated the NIH program focused on COVID-19 in children that the NICHD leads. It is the Prevail Kids program, which is part of the overall RADx Radical initiative, not RADx Radical.
Related: