Last year, 16-year-old Emma Mills developed a migraine headache that lasted for months. Saddled with constant pain, she struggled to attend school, do her homework or spend time with family or friends.
“She missed almost half a year of school. It just really affected every part of her life and our lives,” her mom, Kate Mills, 46, of Raleigh, North Carolina, told TODAY. “The more school she was missing, the more stressful it became and it compounded the headaches.”
About 10 percent of children and nearly 20 percent of teens experience migraine headaches, according to Johns Hopkins Medicine, and they can begin in early childhood: the average starting age is 7 years old for boys and 10 for girls.

For Emma, sometimes the pain felt so intense that she could only lie in a dark room and wish for relief. After trips to urgent care, two stays at Duke Children’s Hospital and Health Center and numerous interventions, her family said, Emma started seeing a cognitive behavioral therapist and physical therapist to help relieve the tension in her head and neck.
When the pain feels severe, her mom said she takes a combination of drugs to reduce the intensity of the headache.
“It has been a process and an evolution. It has been a character builder and it has given her more empathy for others,” her mom said. “She has a good heart and tries to find a silver lining.”
For many children and teens with migraine, finding relief can be challenging -- and the condition isn't always recognized.
As new research has been released over the past 15 years, doctors now have a better understanding of how to help children with migraine.
The first update to the guidelines for treating children and teens with migraine since 2004 has just been released by the American Academy of Neurology and the American Headache Society.
“Healthy habits and a multi-pronged approach can work,” Dr. Andrew Hershey, endowed chair and director of neurology, director of the Headache Center at Cincinnati Children’s Hospital Medical Center, and an author of the guidelines, told TODAY. “It demonstrated and expanded our clinical experience that NSAIDS (nonsteroidal anti-inflammatory drugs) and triptans work in children.”
The recommendations include:
- Making sure patients undergo an in-depth medical history and physical examinations, including one with a neurologist or headache specialist.
- Relying on cognitive behavioral therapy with amitriptyline to reduce frequency of migraine.
- Encouraging enough sleep, regular eating and proper hydration.
- Using ibuprofen, triptans and combination sumatriptan/naproxen during an attack to ease pain.
- Avoiding Botox, which can work in adults, but isn’t effective for children and teens.
These new recommendations reinforce what experts suspected about managing migraine in children and teens, Dr. Christopher Oakley, director of the Johns Hopkins Pediatric Headache Center said.
“It is not a dramatic change, it takes it a little further and gives us a little more evidence,” he told TODAY. “(They have) given us a few other treatments.”
How lifestyle changes make a difference
Jamie Davis Smith’s son Ben started getting migraines when he was 10 and needed to get a “cocktail of migraine medications” to stop the pain. He missed 15 days of fourth grade because of headaches that lasted for days.
“My son really suffered until we got a good treatment plan in place,” Davis Smith, 44, an attorney in Washington, D.C., told TODAY, via email.
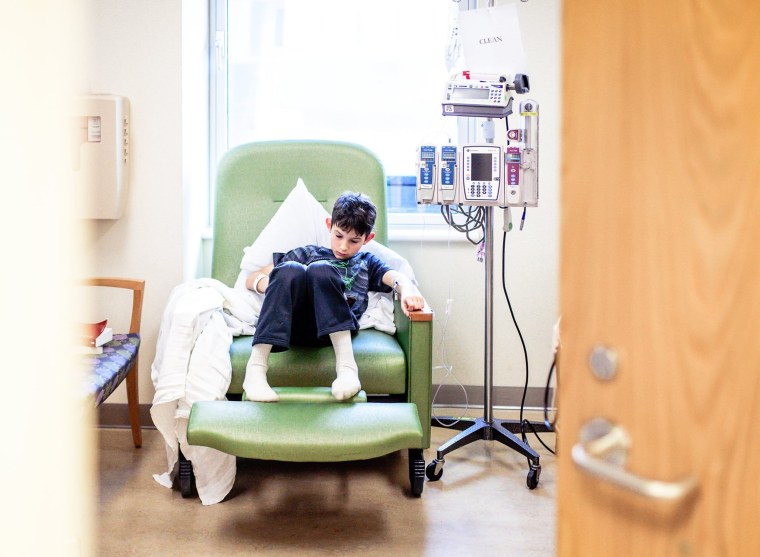
His new doctor recommended lifestyle changes. For example, he said Ben, now 11, should drink Gatorade as soon as he feels an aura -- a sensation preceding migraines that might include light or sound sensitivity -- coming on. These changes have made a huge difference for Ben, the family said.
“We try to stay on top of it,” Davis Smith said. “I do notice that if my son doesn’t drink enough or goes to bed late a few days in a row, he will get a migraine.”
Regular meals, a good night’s rest and proper hydration work because the brain needs fuel. Without it, blood vessels dilate, which can lead to the severe headache pain.
“Healthy habits are the mechanism that allow the brain to compensate,” Hershey said. “The brain is really stressed by dehydration or not getting meals or not getting enough sleep."
School or home stress can be connected to migraines
Another lifestyle change, cognitive behavioral therapy (CBT) works well for many patients, like Emma, because it helps them learn to manage pain. It also provides strategies they can use to grapple with migraine triggers, such as the start of school or a big test.
“We do know that stressors -- difficulty with school or at home, psychosocial things -- can negatively impact migraine,” Dr. Ann Pakalnis, director of the pediatric headache clinic at Nationwide Children's Hospital, told TODAY. “(In CBT) you are working on lifetime coping skills.”
Patients report more headaches on Mondays or at the start of the school year than other times. Stress certainly plays into that, which is why having coping mechanisms can help.
“We highly recommend, if their children are very prone to the stress and anxiety of school, they try to get into a cognitive behavioral therapy or bio-feedback before the start of the school year. If the school year starts and they don’t get off to a good thing, they are missing school and their grades suffer,” Pakalnis explained.
Emma has slowly returned to school, had a job and organized a book drive for the children’s hospital where she was treated this summer.
“The behavioral therapy was great,” Mills said. “(It) helped her see that she could still reclaim her life and be in control of it. The pain wasn’t in control.”