The last person you would expect to come forward about a bowel disease is a former beauty queen — but that's exactly what happened earlier this month when former model and Miss Scotland finalist, Paula O'Neill, spoke out about suffering from ulcerative colitis.
O’Neill said her appearance was so changed by steroid medication that she had to give up modeling. Her weight fluctuates frequently and medications have caused her cheeks to swell, resulting in a common side effect referred to as "moon face."
“People who know me didn’t know what to think,” she told Scotland’s Sunday Post. “I’m sure some of them thought, ‘Paula’s really let herself go!'" In reality, O'Neill noted that the side effects are a price worth paying for medication that helps her feel better.
Though it might be a condition rarely spoken about, an estimated 1.6 million Americans suffer from inflammatory bowel diseases like ulcerative colitis and Crohn’s disease, according to the Crohn’s and Colitis Foundation of America.
RELATED: 'I wasn't ashamed': Woman with Crohn's disease shows off colostomy bags in stunning photo
These diseases usually strike before the age of 35 and tend to run in families.
Amber Elder was so embarrassed about her chronic diarrhea and rectal bleeding that she couldn’t even share her increasing health problems with her mother.
“No one talks about their bowel habits,” said Elder, a 32-year-old blogger from Shreveport, Louisiana. “Who really wants to talk about poop?”
Elder was in the bathroom at least 20 times a day and was unable to travel because she had accidents on the way to work.
“It was a complete nightmare,” she told TODAY. “There were nights I sat on the bathroom floor crying over the toilet.”
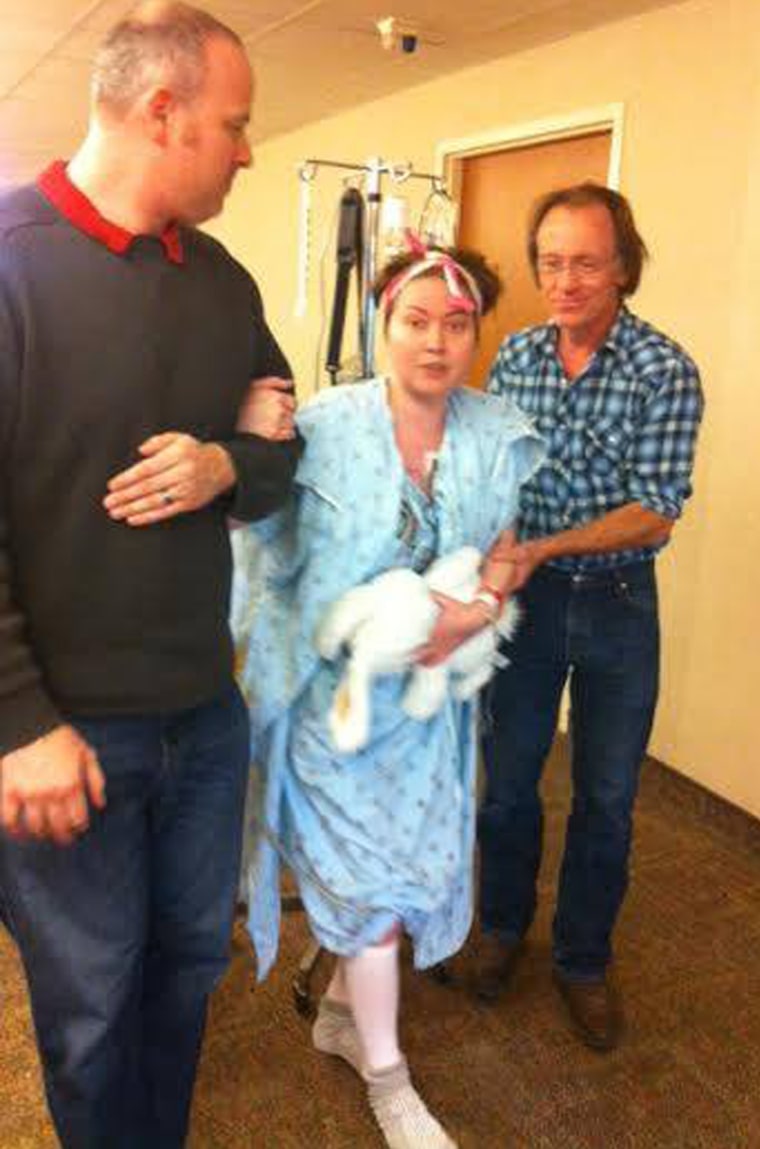
By 2011, Elder had such severe abdominal pain, she was sent to the emergency room and diagnosed with ulcerative colitis, an incurable autoimmune disease that affects the colon.
RELATED: 'Invisible illnesses need more awareness': Viral photo sparks important discussion
“I was 26 and thought I was invincible,” she told TODAY. “I was a student of karate and was only six months away from getting my black belt when the disease hit and threw me for a loop.”
Today, Elder is in remission and has overcome feelings of shame. She blogs as the Colitis Ninja, raising awareness and support for patients and caregivers.
“It’s so isolating,” said Elder, who adds she delayed seeking help because of the taboo surrounding the disease. Doctors often confuse symptoms with the more benign irritable bowel syndrome. Her then boyfriend, who is now her husband, even accused her of being a “hypochondriac.”
RELATED: Bloated belly? Why your hormones might be the secret cause

Surprisingly, Elder later learned her mother and an aunt suffered from Crohn’s disease, which affects not just the large intestine, but the entire gastrointestinal tract.
Initial treatment with steroids caused Elder to have debilitating side effects: joint pain, hair loss, mood swings and, like Paula O'Neill, “moon face.”
“You don't recognize yourself anymore,” said Elder. “What makes it worse is you don't feel like yourself. It's almost like you lose your identity because ulcerative colitis robs you of so many things.”

Elder endured two surgeries in 2014 to remove her colon and to build a so-called “J-pouch,” a reconstruction of the small intestine, which acts as a colon and stores fecal matter.
Inflammatory bowel diseases are rarely fatal, but they're challenging because of the “terrible” symptoms, said Dr. Scott Snapper, director of the inflammatory bowel disease center at Boston Children’s Hospital and associate professor at Harvard Medical School.
“Any GI disease is difficult for a patient to even talk about,” Snapper told TODAY. “And not just with doctors, but they are hesitant to talk with anyone.”
RELATED: 'I thought it was an old man's disease'
“When someone is at work and they have to go to the bathroom five or 10 times a day in a flare-up, the tendency is to think of the person as a whiner," he said.
Treatment depends on the severity of the disease and how an individual patient responds to medications. Some will only need a topical enema; others may require oral anti-inflammatories.
Immune modulators, biologic drugs or anti-trafficking agents that block the movement of white blood cells, are also used when other medications fail or patients do not respond fast enough, said Snapper.
Patients like Elder, who require surgery, often do “very, very well,” said Snapper.

Steroids are used when there is a flare-up of the disease and may be used in conjunction with other therapies.
“But steroids are never desirable for long-term treatment because of the complications on many organs,” said Snapper. “Moon face is one; (also) high blood pressure and eye and bone issues.”
Snapper, who also chairs the national scientific advisory committee at the Crohn’s and Colitis Foundation of America, says research is “making tremendous progress.”
“Many, many patients lead normal, healthy, productive and romantic lives,” said Snapper.
Such is the case with Amber Elder, who married the same year she was diagnosed with ulcerative colitis.
“To patients, I say advocate for yourself and make sure you take control of your health and find support,” she said. “And to caregivers, be patient with us. At least try to understand what we are going through and support us.”