Doctors hate to use the word, “miracle,” but in Cristina Beltran’s case there’s no other way to describe how she is still alive. So many things had to go just right, not the least of which is the good fortune to have found a doctor who figured out a medical condition no one had ever heard of.
In 2011, Beltran, 24, was living her dream. She’d moved to New York City from California and was rooming with her best friend from college, Lizzie Ross. “We were excited to live in New York and get going with our lives,” Beltran, now 28, told NBC News national correspondent Kate Snow as the final part of the TODAY series, "Medical Mysteries".
But after a weekend away with friends, the unthinkable happened: Cristina’s heart stopped beating.
Beltran and Ross had been unpacking in separate rooms. “I heard just a really bad noise, a gasping for air,” Ross said. “I ran into Cristina's room and she was on the ground face down, blue. It was really scary.”
By an amazing bit of good fortune, Ross had just been certified in CPR and went right to work. The last thing Beltran remembers is her friend asking, “so what do you want for dinner?”
“And suddenly three days later I woke up in the hospital,” she said.
Ross called her friend’s parents, who rushed to New York, to their daughter’s side.
The doctor told her mother, "'The survival rate for cardiac arrest outside of the hospital is 7.9 percent. And if she’s in a vegetative state when she wakes up, we will not keep her alive,'" Lina Beltran said.
Once again, Cristina Beltran beat the odds. She was out of the hospital in little more than a week.
“I remember my doctor saying it was one of the quickest recovery times anyone had ever stayed after a cardiac arrest,” Beltran said.
It didn’t last. Just months after her initial heart stoppage, Beltran began to feel chest pains. Doctors did an angiogram and saw blockages in her arteries that looked like plaque.
But it didn’t make sense that a fit and otherwise healthy young woman would have blocked arteries.
“There was no family history,” said heart specialist Dr. Hooman Yaghoobzadeh, a clinical professor of medicine at New York-Presbyterian/Weill Cornell Medical Center. “Her cholesterol was normal; there was no substance abuse; she didn’t smoke; she wasn’t diabetic. But she had the blood vessels of a 75-year-old hypertensive, diabetic smoker.”
Even if the baffled doctor didn’t understand why it happened, he still needed to do something to prevent another cardiac arrest. Beltran's narrowed arteries were forced open with stents, thin tubular scaffolds that are placed inside a blood vessel and then expanded with a balloon. But the stents were only a temporary fix.
Beltran’s arteries started narrowing where they weren’t stented. At age 25, she was told she needed triple bypass surgery.
“I remember the doctor saying, ‘we need to do surgery,’” she said. “And I started to cry.”
During the surgery Beltran’s doctors biopsied her blood vessels, which offered an important clue: her arteries weren’t clogged with plaque. Instead, the lining of the blood vessels had grown so thick that it essentially was closing them down.
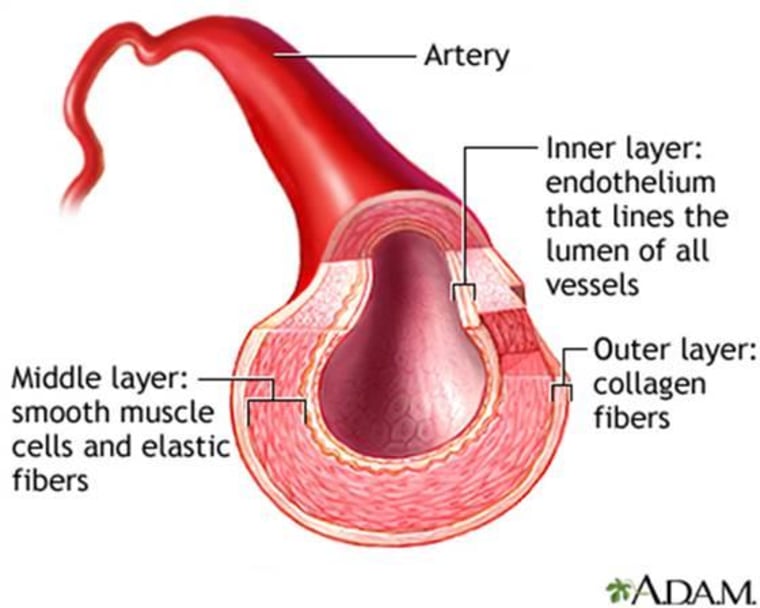
Yaghoobzadeh had a hunch how to fix it. Beltran’s arteries had narrowed only at the front of the stents but not at the other ends, which were coated with a medication called rapamycin. Rapamycin had been used in heart transplant patients whose bodies had started to reject the organ. The rapamycin calmed down the inflammation that had developed in their arteries and allowed them to open up.
The drug worked better than Yaghoobzadeh could have hoped for.
But the doctor and his patient still didn’t know why all this had happened. The answer would eventually come from genetic tests done on Beltran and her parents. As it turned out, both her father and her mother carried a mutation and Beltran got both copies.
“The [defective] gene that she’s gotten from her mom and her dad is a blueprint for the muscle cells in the arteries of her heart,” Yaghoobzadeh said.
Choosing to treat Beltran with rapamycin “was a shot in the dark,” Yaghobzadeh said. “We hit on a drug that seems to be very, very active in the exact pathway that is affected by her genetic abnormality. And thankfully we started treating her six months before we knew what that abnormality was. I think those six months made a big difference.”
Beltran’s genetic mutation is rare, but not so rare that there wouldn’t be people out there with just one copy—or even two, like she has, Yaghoobzadeh said, adding that one copy might be enough to cause early onset heart disease.
That’s why Yaghoobzadeh and scientists at the National Institutes of Health are looking for people like Beltran—people who, at a young age, might have had a cardiac arrest or angina. They suspect that two patients might teach them a lot about how heart disease develops even in people without the mutation. [If you suspect you may have the condition, or know someone who does, you can contact Yaghoobzadeh at Dryaghoobzadeh@gmail.com.]
As for Beltran, she’s taking a number of medications, but otherwise seems to be in perfect health. She now works in fashion and chronicles her life in a popular blog, no longer worried about what the future will bring.
Read more about Cristina's story at her blog: http://www.theresidenttourist.com/
Kate Snow is a national news correspondent with NBC News. Linda Carroll is a regular contributor to NBCNews.com and TODAY.com contributed to this report. She is co-author of "The Concussion Crisis: Anatomy of a Silent Epidemic” and the recently published “Duel for the Crown: Affirmed, Alydar, and Racing’s Greatest Rivalry”
This article was originally published Mar. 6, 2015 at 9:23 a.m. ET.