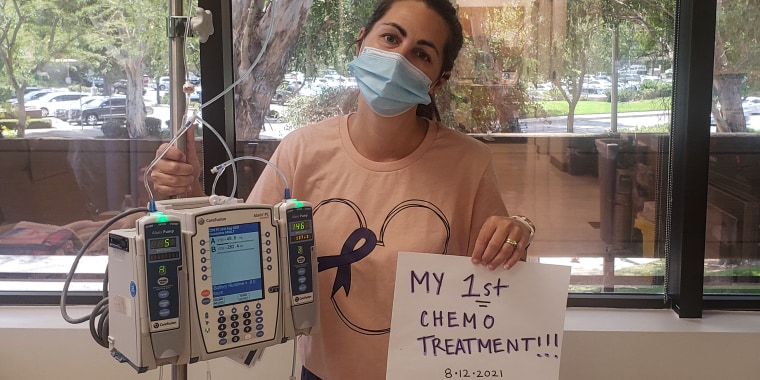The contraction-like pain shot across Melissa Ursini’s lower abdomen for an hour at a time. It would subside, then come back. She scheduled an appointment with her OB-GYN, but tests results looked normal. Still, her symptoms didn’t improve. At one point, she was told she had a parasite. Then learned what was wrong: She had stage 2 colon cancer.
“I wasn’t losing weight. I was still exercising when I wasn’t in pain,” Ursini, 38, of Santa Clarita, California, told TODAY. “The thought of colon cancer never hit my mind. I actually thought if it was any cancer it would have been ovarian cancer … or breast cancer.”

Ursini is one the nearly 18,000 people under 50 diagnosed with colon cancer in a year, according to the American Cancer Society.
“I’m hoping that people realize it’s not an old person’s disease,” she said. “It’s becoming more common for younger people to get colon cancer. Don’t balk reading those symptoms of abdominal pain or if you see blood in your stool. Got to the doctor, go get that checked out.”
Stomach pain, loss of appetite, vomiting
In June 2021, Ursini started experiencing stomach cramps that felt like labor pains. After her OB-GYN conducted a few tests and ultrasounds that appeared healthy, Ursini visited a gastrointestinal doctor. Between appointments, her symptoms worsened.
“Every couple minutes I had this big shot of pain go across the lower abdominal area and then it would go away and then it would come back and then it was stable,” she said. “It grew from there.”

The pain became constant like period cramps and her appetite had waned. But she wasn’t losing any weight even though she was eating less. While the GI doctor scheduled her for a CT scan with contrast, she started to have terrible stomach cramps and began vomiting. She thought it was a reaction to an antibiotic so she visited the emergency room.
“The doctor dismissed it a little bit and he’s like, ‘I think you’re constipated’ and I was like, ‘Well I haven’t really eaten anything. Everything coming back up,’” she recalled.
The doctor ordered a CT scan without contrast and it looked clear.
“We didn’t see the tumor,” she said. “We thought it would be like irritable bowel syndrome.”
By this point, Ursini felt constant pain. Again, she started throwing up and returned to the emergency room.
“The doctor came in and goes, ‘I know what you have, you have a parasite. Have you been traveling?’ and I’m like, 'Not really it’s COVID. I haven’t traveled. I’ve literally been at home,’” she said. “He gave me an antibiotic.”
By this point, Ursini was throwing up so much she felt grateful for days when she didn’t. Then one night, she started vomiting bile.
“It smelled,” she said.
She called her brother-in-law, Hector Leanos, an ER nurse. He suspected she had an obstruction.
“He goes, ‘Does it smell?’ I said, ‘Yeah.’ He said, ‘I don’t care what you’re doing I will come pick you up … you need to come to my hospital,’” Ursini said. “(He said) I’m going to let them know because I think it’s an obstruction.’”
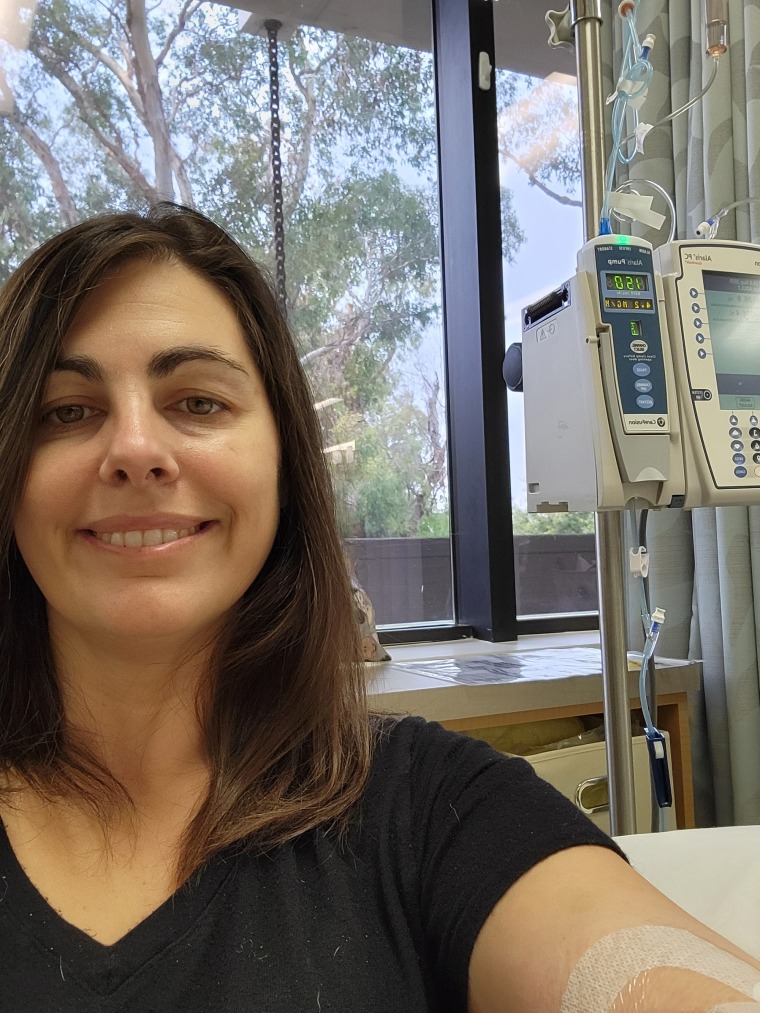
After several tests, including a CT scan with contrast, the doctor delivered the news that it was colon cancer. At first, Ursini didn’t grasp the news.
“There was a mass inside my intestines causing me to back up,” she said. “Never in my mind would I ever think I had cancer.”
She underwent an emergency colonoscopy, which only reached the mass. She underwent surgery where they removed the mass, 7 inches of intestine and tested 56 lymph nodes for cancer.
“I was in shock,” she said. “Everything doesn’t add up.”
Her father had non Hodgkins lymphoma and lost weight and had abnormal bloodwork. That never happened to her. While her grandfather had died of colon cancer, her mother's cancer screenings never detected anything.
“They found (my grandfather’s cancer) so late that when they went in for surgery, they opened him up and then within 10 minutes came out and said, ‘There’s nothing we can do,’” she said. “You can imagine what my mom was going through when I went in for the same surgery almost 40 years later — she kept imagining they were going to come up and say the same thing.”
Colon cancer in young people
Once considered an older person’s cancer, doctors have noticed that more young people are being diagnosed with colorectal cancer.
“The risk of colorectal cancer does increase with age and it used to be an older person disease,” Dr. George Hajjar, a medical oncologist and hematologist at City of Hope and one of Ursini’s doctors, told TODAY. “Over the last 22 years of my career I (am) seeing that younger people are getting early disease and we are really not sure what’s causing it.”
People with a family history are at a higher risk and undergo screening about 10 years earlier — at 35 instead of 45 for people without a family history. Ursini’s cancer did not have a genetic component but even still her daughter would qualify for earlier screening.
“It’s very important when we meet patients to get a good family history of malignancy because that might give us a tip to start screening early,” Hajjar said.
Symptoms of colorectal cancer include:
- Rectal bleeding
- Anemia
- Abdominal pain
- Changing bowel habits, including diarrhea or constipation
- Feeling full sooner
Symptoms can be “nonspecific,” meaning they are common enough that they could indicate other conditions.
“Who would think that they will have colorectal cancer if they have some abdominal discomfort or change of bowel habits,” Hajjar said. “That’s where the screening idea came from.”

Treatment varies based on the stage but most people undergo surgery to remove the tumors and any cancerous lymph nodes. Sometimes follow up with chemotherapy is needed and patients will be followed closely after they complete treatment for the first few years. As for Ursini, her outlook seems promising.
“She brought it to our attention at the right time and she had the appropriate treatment,” he said. “She did everything right.”
Life after treatment
Treatment felt tough at times. Ursini lost some hair, struggled to sleep and experienced neuropathy that made her extremely sensitive to cold. She skipped drinking iced tea and sometimes she couldn’t touch cold things because it caused pain.
“I would go to the grocery store and I would have winter gloves on because if I touched something (cold) it would hurt so much,” she said. “I was pretty lucky and I don’t think the side effects were as bad as they could have been.”She finished treatment in October and follow-up scans and a colonoscopy show she’s cancer free. She feels grateful for her health.
“My body has taken me very far. First, it helped grow me so I’ve grown in this body but I’ve also grown a human. I grew cancer. I got that cancer removed, went through treatment,” she said. “There are times when I took this body for granted by not being happy with weight loss or pushing it a little too far with exercising or not eating the right things … This body has taken me far and (it’s) going to take me even further.”