Viral encephalitis is an inflammation of the brain caused by a virus or infection, or autoimmune conditions. The most serious potential complication is permanent brain damage. Encephalitis is relatively rare and the condition more often occurs in younger people, according to Johns Hopkins Medicine.
As I prepare to run my second New York City Marathon on Nov. 6, 2022, I’m sharing my story to raise awareness of this serious brain infection, as well as the relationship between neurological recovery, fitness and brain health.
I remember how amazing it felt the moment I crossed the finish line at my first New York City Marathon on Nov. 7, 2021. I can’t recall ever feeling so confident and ready for anything that might come my way. I knew how hard I had trained and how committed I was to completing this race. It was probably one of my proudest moments.
From the March 2020 shutdown due to COVID-19, my life revolved around staying healthy, staying positive and running. To stay balanced as the world seemed to unravel, I ran. I ran 20 virtual and in-person races in 2020, followed by even more races in 2021. Last New Year’s Eve, I ran a race in Central Park with fireworks — we all literally ran into the new year. I felt like I was starting 2022 on the right foot, but sometimes life takes an unexpected turn.

In early January, I could not shake the cold and flu symptoms I had been having. My doctor told me to go to the emergency room. They gave me fluids and sent me home. The next day, I was even worse. My parents came to my apartment and took me back to the ER. Everything went downhill from there. I had a fever and headache and was vomiting. I had terrible pressure in my head that felt like it was going to explode. My mother noticed that my speech was slurred. My vision was blurry, I was drooling and couldn’t swallow. The last thing I remember is a young ER doctor suggesting a spinal tap. Once the procedure was done, I went into a coma.
The last thing I remember is a young ER doctor suggesting a spinal tap.
I was transferred to the neurological intensive care unit, where I was put on a feeding tube and ventilator. While unconscious, I was also diagnosed with COVID. My parents said that the doctors overseeing my treatment were evasive and noncommittal about my recovery, but they did not give up hope. Family and friends were all praying for me.
When I regained consciousness approximately two weeks later, I was terrified. I could not speak, breathe on my own, eat or walk. I was connected to so many machines and heard constant beeping noises. I was so weak I could barely move, and I was in a lot of pain. All I could do was cry. I eventually was told that after multiple MRIs, CT scans and blood tests, I tested positive for enterovirus and was diagnosed with viral encephalitis, a rare brain infection that almost ended my life. The doctors were able to treat me with intravenous immunoglobulin (IVIG) infusions, which saved my life.

Most treatments for encephalitis focus on rest, nutrition and fluids to help the body fight the infection and relieve the brain inflammation. It was crucial for the doctors to lower my fever and ease the pressure caused by the brain inflammation. Some of the treatments aimed at reducing my symptoms included steroids to reduce brain swelling, anticonvulsant drugs to prevent seizures and sedatives to calm me down.
My neurologist came to check in on me every day and provide updates, but I was in a fog. I felt like I was living in a nightmare. How and why did this happen to me? I felt that my life as I knew it was over. I was in so much pain and I couldn’t move. When visiting hours were over and my mother or father had to leave, I lay there for hours feeling so alone, hopeless and despondent.
To communicate, I had to use a laminated folding card with the letters of the alphabet printed on it. I eventually had enough strength to point to each letter to spell out words and sentences to get my thoughts across to doctors, nurses and my parents. It was so difficult and frustrating. I wanted to do everything within my power to regain my strength, but there were some challenging and dark days when I just wasn’t sure I could. Every day was a struggle, not knowing what my future would look like. There were no clear answers. I was being poked daily with needles and being fed through a feeding tube up my nose.
When the doctors took me off the ventilator, they had no choice but to perform a tracheostomy, a surgically created hole (stoma) in your windpipe (trachea) that provides an alternative airway for breathing. I eventually learned how to speak with the “trach” in my neck with a little device that I’d screw on, a “speaking valve,” which was still painful to do since air was coming into and out of my mouth and the trach hole in my neck.
At night I would practice talking with the man who would remove the wastebasket in my room. We became friends. I looked forward to his visits. Whenever he was on duty, he would make an extra effort to visit me and stay a bit longer each time, just talking. One night he told me his entire family was praying for me.
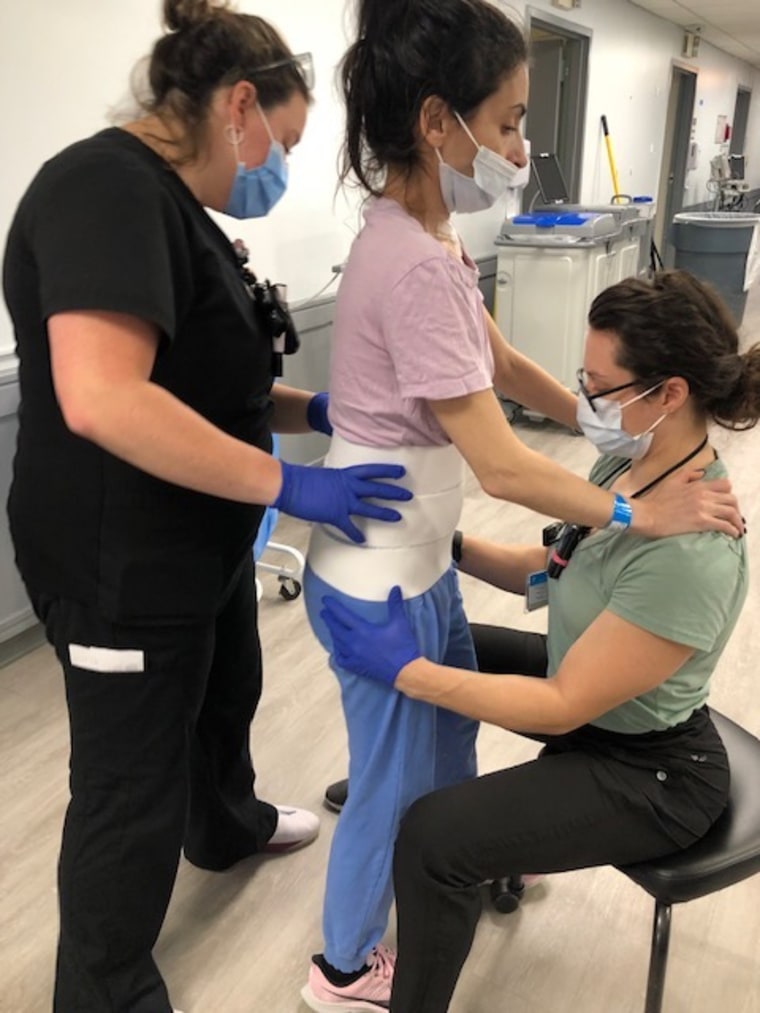
I started recognizing the nurses. Getting to know them was a way for me to start feeling like a normal person again. It also was good practice using the valve on the trach to speak. Talking became a workout, just trying to get words to come out. Some of the old-school nurses gave me tough love — they pushed me to try to do things on my own when I didn’t think I was strong enough. Another nurse would joke around with me all the time. I started to feel I might be getting better.
For two months, I lay there at Mount Sinai Hospital in what felt like a prison cell. I still couldn’t do anything on my own — I was always depending on someone else to help me. I didn’t have any strength in my arms or legs, could barely swallow anything, and my whole body felt sore from laying in bed 24 hours a day.

As despondent as I was, my doctors were amazed at my progress. When I was finally strong enough to be accepted into the hospital’s acute rehabilitation center, I was treated by specialized neuro-physical and occupational therapists. I started to walk in less than a week. The version of myself I was once so proud of was coming back to me, and it felt exhilarating. After just 13 days in acute rehab, I could walk on my own, using a cane for support and balance. I was finally discharged from the hospital.
Survivors of encephalitis can suffer neurologic consequences, which can be long-term and even permanent. The location and severity of the infection largely determines the pattern of brain damage and its effects, which, according to Mount Sinai, can be physical (muscle control); behavioral and emotional (personality changes); cognitive (memory, speech) and sensory (vision, hearing). It was critical for me to initiate physical therapy, speech therapy and occupational therapy.
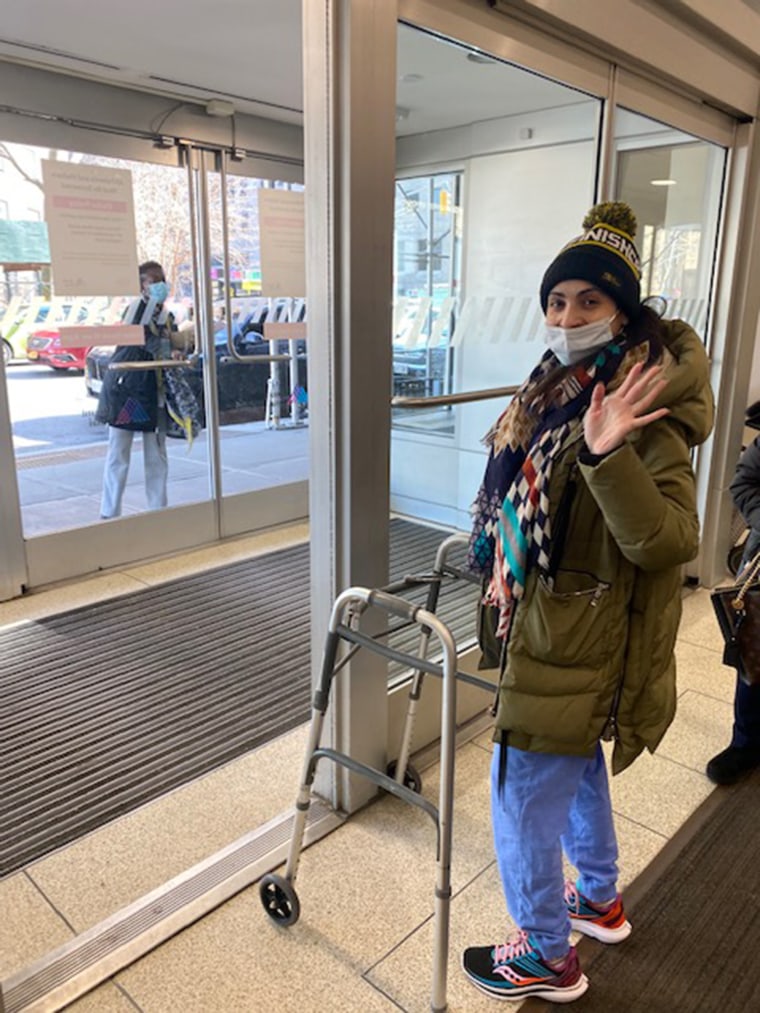
Even after all these months, I still feel fatigued after physical exertion.
I’ve now been out of the hospital for more than seven months. I feel grateful to be alive. I’ve learned to walk without assistance, and now I can even run. I can eat, speak and do all the basic, daily life tasks that so many of us take for granted. The one lingering ailment that I still deal with today is my speech. I have neuropathy (nerve damage) in my tongue that makes it feel like my tongue is in the way, and it impairs my speech. But it has been improving daily (at least that’s what my friends, family and doorman say). I have made gradual, steady improvement and my recovery has far exceeded everyone’s expectations. I started running short races — 5Ks as well as a four-mile race earlier this summer. Getting to the finish line was a great feeling. I can’t change what happened to me, but I can change my perspective and appreciate how far I’ve come.
I’ve been training for my second New York City Marathon, and now I'm finally ready. I’ve been given a second chance at life — a full and fulfilling life that I plan to embrace and enjoy every moment moving forward.