In the midst of coronavirus-fueled chills, fever and diarrhea, Dr. Chadi Hage stumbled across a request for researchers to lead clinical trials examining COVID-19 — he applied, and now he’s heading two COVID-19 studies. Hage believes that his experience as pulmonologist, and a person who had the coronavirus, makes him well suited for the task.
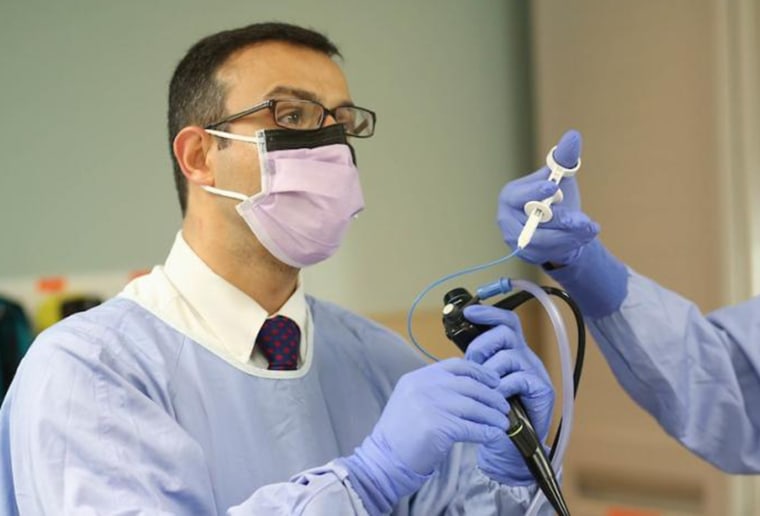
“You become more respectful of the virus and the effect it has on people,” Hage, an associate professor of clinical medicine at Indiana University School of Medicine, told TODAY. “Having gone through it, I can tell you this is a serious infection for someone who is healthy otherwise and has no underlying medical conditions whatsoever.”
From infection to investigation
At the end of March, the chills, fever and diarrhea began and Hage immediately suspected it was COVID-19. At the time, not everyone was required to wear masks all the time, though fortunately the policy has changed, he added.
“It starts with headache and fever and diarrhea and dehydration,” he explained. “I didn’t have respiratory (symptoms). It was mostly fever and chills.”
The headaches lasted for about three days before the fever, diarrhea and chills began. The fever lasted for 11 days in total. Still at first, he didn’t feel too sick.
“The funny thing about this disease is you get better initially and then a week later, it gets much worse. And that’s the immune response,” he said. “You get the initial infection and then you feel bad and everything, almost seven or eight days, the symptoms take it to another level. It gets much worse and that’s scary."

While he isolated as soon as he felt ill, his wife and daughter still contracted COVID-19 (though both had much milder cases than Hage who says this follows the trend found in the literature that men have COVID-19 more severely than women).
“When I started having symptoms we separated into different rooms. But it was too late,” he said. “As we now know, you’re contagious before you have any symptoms.”
Towards the end of his illness, Hage applied for the clinical trials, which both focus on better understanding the inflammatory response to COVID-19.
“For one reason or another the response is very intense, a cytokine storm. This is what makes people so sick,” he explained. “The patient’s viral load is actually on the way down when the patient’s getting worse. So it’s not really that you have more virus in your system. It’s the virus on its way out.”
But the immune system mounts an “exuberant” response at this time, which is often about a week after symptoms start. The studies Hage leads are looking at therapies to slow the overreactive system.
“The thought behind them is the fact that if you medicate this exact exaggerated immune response to make people less ill they therefore recover faster,” he said. “We will probably need a multi-pronged approach to medications that will affect the virus directly.”
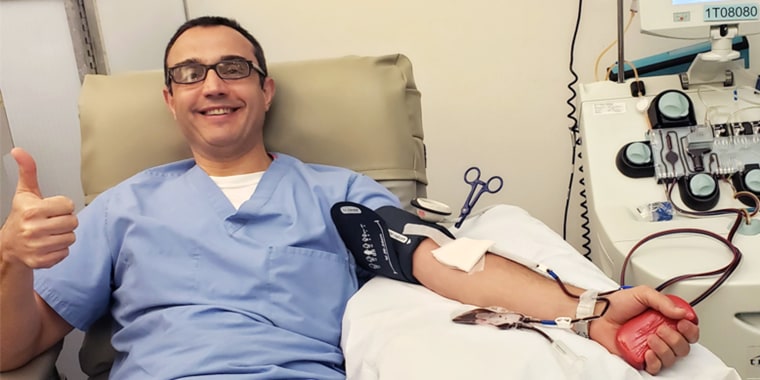
Even though Hage knew it would take time to fully recover after having COVID-19, he tried to test his strength after he went four days without symptoms. The long- distance cyclist hopped on his bike and set off. But he soon found himself struggling to complete 15 miles, a ride that wasn’t challenging prior to him becoming ill.
“I was exhausted. I didn’t think I was going to finish. And, I normally do a lot more than that,” he said. “It took me a while to recover my strength and endurance.”
About two weeks after that ride, he estimates that he was 80% of his normal ability and now he feels back to normal.
“It has taken a while to get there,” he said.
While he hopes that the trials will lead to better treatment, he really wants people to understand that COVID-19 is dangerous, even for people who don’t end up in the hospital. He encourages people to wear masks, wash their hands frequently and social distance.

“This is not a political game. This is serious stuff. People die from COVID-19 and we really have to do our part to control it,” he said. “We have to rely on the science.”