Soon after Barrett Williams was born, his parents learned he had a congenital heart defect. While he had a procedure at 2 months old to help, his parents knew he’d need to undergo open-heart surgery someday.
“We knew that one day eventually he would most likely need to have his aortic valve replaced,” mom, Joanna Williams, 41, of Park City, Utah, told TODAY. “We just hoped we could prolong it for as long as possible.”
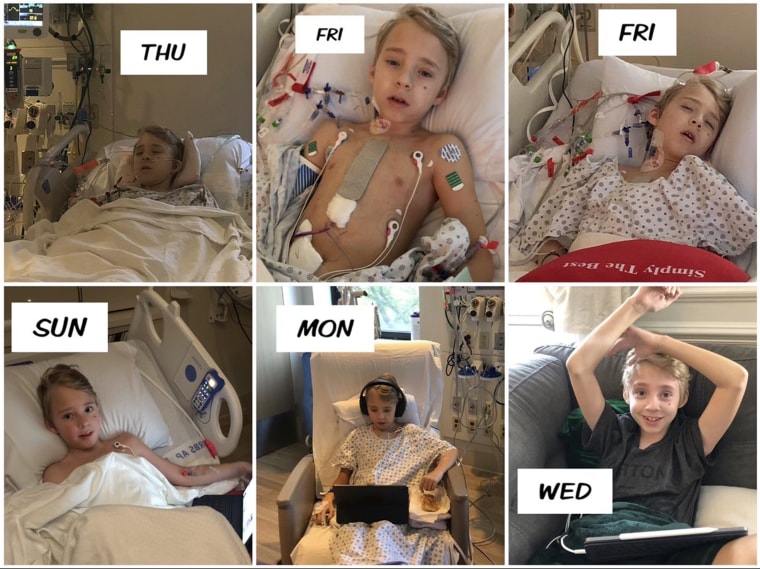
Barrett's heart defect didn't hold him back — he was able to participate in activities any other young child would until last summer. His condition worsened, and his family learned they needed to prioritize surgery. They worried about Barrett, now 10, undergoing such a serious operation in the middle of a pandemic. But thanks to a special surgical procedure, Barrett is home, healthy and hitting the ski slopes.
“It’s just shocking to me how quickly he recovered,” Williams said. “It was pretty amazing.”
Congenital heart condition and open-heart surgery
Congenital heart defects (CHDs) are the most common type of birth defect, affecting nearly 40,000 births in the U.S. each year. According to the Centers for Disease Control and Prevention, 1 in 4 babies born with a heart defect has a critical CHD and will need surgery.
When Barrett was born, he had aortic stenosis and a unicuspid valve, resulting in issues with blood flow in the heart. While the procedure he had done as an infant opened up his valve, it wasn’t a permanent fix.
“What happens in people born with a unicuspid is that the valve starts to malfunction earlier in life and so patients typically need surgery in their teens or even their 20s,” Dr. Ismail El-Hamamsy, who treated Barrett and is the director of aortic surgery at Mount Sinai Health System in New York, told TODAY.
That’s what happened to Barrett. He developed regurgitation, meaning that some of the blood pumped out of the heart chamber leaked back into it. Without treatment it could lead to heart failure. Luckily, Barrett hadn’t experienced any problems yet.
“I didn’t realize anything was wrong,” Barrett told TODAY. “I was maybe a little out of breath.”

But his parents wanted to act before he worsened: A routine MRI showed that his regurgitation had reached a "significant point," Williams said.
She had been researching treatments and thought Barrett would do best with what’s known as a Ross procedure, which uses the patient’s own pulmonary valve to replace the aortic valve and a cadaver valve to replace the pulmonary valve. It’s often a good option for children because if they receive a mechanical valve, they have to take blood thinners for their whole lives.
“For someone who is young and active and wants to play sports — whether it's contact sports or things like skiing where you're at risk of falling and knocking your head — you have a much higher risk of major bleeding (from taking blood thinners),” El-Hamamsy said. “We want to balance doing the surgery that will allow him to have a good quality of life.”
Though, not every doctor performs such a surgery and Williams struggled to find someone close to home who could do it.
“This meant going out of state,” Williams said.
She and Barrett had to travel to New York City for El-Hamamsy to perform the Ross procedure. The logistics felt overwhelming at times.
“It was definitely tricky,” she said. “The first thing was to get all of his records, all of his echocardiograms and the office notes, sent. But a lot of the records departments were closed.”

They also had to be extra careful not to catch COVID-19 during travel. Only one parent could be at the hospital for support and Williams worried.
“It was pretty nerve-wracking to be the only one parent,” she said. “What if something happened? What if I got sick? What if I got a fever and they wouldn't allow me in the hospital, and I'm the only person there? That was something that was really I was really worried about.”
While open-heart surgery sounds scary, Barrett initially wasn't intimidated.
“When it was getting closer to the surgery, I started to get a lot more worried,” Barrett said.
Williams and Bennett flew to New York in September and he underwent the surgery.
“It was rough the first couple of days,” Williams said. “After day two, I was just surprised how quickly how quickly he improved.”
The first few days remain a blur for Barrett, but he felt better than expected.
“The third, fourth day, I started … to snap out of it,” he said. “The scar’s actually a lot better than I thought it would be.”
After two weeks, Barrett returned to home to continue his recovery.
“Once we got back, I was kind of getting back into the swing of things,” he said. “I feel perfect.”
Life after open-heart surgery
After Christmas, doctors allowed Barrett to resume his normal activities. Since then, the fifth grader has gone skiing about a half dozen times. He looks forward to warmer weather where he can ride his mountain bike again without having to worry.
“I feel really good,” he said. “I love skiing.”

El-Hamamsy said the surgery gives Barrett the chance to be like any other kid.
“It is the only replacement operation that allows us to restore life expectancy of these patients to that of the general population,” he said. “There's no medication that is required. There are no limitations to what he can or cannot do. It’s a perfectly normal quality of life.”
